Strategies to Help Prevent Gout
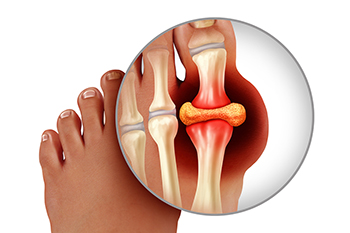
Gout is a type of arthritis caused by buildup of uric acid in the bloodstream. This chemical can build up and crystallize in the joints, particularly the big toe joint, causing sudden and severe joint pain, swelling, stiffness, and inflammation. If you have had a previous gout flareup, or have a family history of gout, learning and utilizing certain prevention strategies can help you avoid future painful flare ups. Consuming a diet low in purines, a chemical found in red meat, shellfish, and other types of food, which is converted to uric acid in the body, can also lower your risk of gout. Staying hydrated by drinking plenty of water can reduce uric acid crystal formation in the kidneys. Losing excess weight, exercising regularly, and avoiding excessive consumption of alcohol and sugary beverages may also help. Certain medications may be prescribed by your doctor to lower uric acid levels in the body. To learn more about preventing and managing gout, please consult with a podiatrist.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Dr. Stephen Petrofsky from Florida. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Port Charlotte, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Everything You Need to Know About Gout
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
Why Do My Ankles Hurt After Running?
Runners take hundreds of steps per minute while they run. During each step, a large amount of force is transmitted through the foot, ankle, and leg. The ankle takes most of the force, so it should come as no surprise that runners often experience ankle pain. There are several factors that contribute to ankle pain while running. Muscle imbalances and weakness or tightness in some part of the foot, ankle, or calf, can change the way force is distributed while you run, putting more pressure on the ankles and leading to injuries. Repetitive overuse from intense bursts of running and not giving yourself enough time to fully recover can also cause or worsen ankle pain. Previous injuries, such as an ankle sprain that hasn’t completely healed or hasn’t healed properly, can increase the risk of future ankle injuries as well. It is important to wear properly fitted, supportive shoes while you run. If you are a runner suffering from ankle pain, it is suggested that you seek the care of a podiatrist.
All runners should take extra precaution when trying to avoid injury. If you have any concerns about your feet, contact Dr. Stephen Petrofsky of Florida. Our doctor will treat your foot and ankle needs.
How to Prevent Running Injuries
There are a lot of mistakes a runner can make prior to a workout that can induce injury. A lot of athletes tend to overstretch before running, instead of saving those workouts for a post-run routine. Deep lunges and hand-to-toe hamstring pulls should be performed after a workout instead of during a warmup. Another common mistake is jumping into an intense routine before your body is physically prepared for it. You should try to ease your way into long-distance running instead of forcing yourself to rush into it.
More Tips for Preventing Injury
- Incorporate Strength Training into Workouts - This will help improve the body’s overall athleticism
- Improve and Maintain Your Flexibility – Stretching everyday will help improve overall performance
- “Warm Up” Before Running and “Cool Down” Afterward – A warm up of 5-10 minutes helps get rid of lactic acid in the muscles and prevents delayed muscle soreness
- Cross-Training is Crucial
- Wear Proper Running Shoes
- Have a Formal Gait Analysis – Poor biomechanics can easily cause injury
If you have any questions, please feel free to contact our office located in Port Charlotte, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Preventing Running Injuries
Over half of all runners encounter at least one injury per year. The reason for this is because many runners do not train properly. Injuries are almost inevitable due to the physical stress that running causes. While our bodies are great at adapting to the stress, it can only handle it in small doses. Injuries occur when the stress is applied too quickly for the body to handle, causing something within it to break down. With each step you take, your leg is absorbing two or three times your body’s weight.
Some of the most popular running injuries are shin splints, plantar fasciitis, Achilles tendinitis, and stress fractures. Shin splints cause pain along the inside or outside of the shins, and this pain is usually felt at the beginning of a run. The condition itself is defined as an inflammation of the muscles or tendons located around the shinbone. To treat shin splints, it is advised that you ice the shin area and stretch the calf muscles. To prevent this injury, you should slowly increase the distance you plan on running, instead of jumping into a more strenuous routine.
Achilles tendinitis is another common injury and it feels like pain along the back of the leg, toward the heel. This condition is defined as an inflammation of the Achilles which is the largest tendon in the body. The Achilles is responsible for connecting your calf muscles to the heel bone and it is caused by tight calf muscles. If you want to treat this injury, you should take a break from running to cross train with a low-impact activity.
There are a lot of common mistakes runners make that are causing them to experience injury. One mistake is stretching too much prior to warming up. If you plan to go on a run, you should warm up with a gentle 3-5-minute walk followed by a 5-minute run-walk. Another common mistake is jumping into a routine too quickly. Consequently, you should incorporate cross-training into your routine. If you are looking to get active, you should slowly weave running into an activity you are currently participating in. For example, you can try bike riding for 40 minutes followed by a 10-minute run.
Another way to prevent running injuries is to choose shoes that are appropriate for running. There are certain things you should look for when buying a new pair of running shoes. An important factor in these sneakers is flexibility. Running shoes should be capable of bending and flexing at the forefoot. However, you should not be able to bend the entire shoe in half with ease because this is a sign that the shoe does not have enough structure. Additionally, you should look for the fit of the running shoes you want to purchase. It is best to visit a specialty running shoe store to have your feet properly sized. Choosing shoes that fit properly can prevent many foot ailments.
If you are suffering from any pain from running injuries, you should make an appointment with your podiatrist to discover the underlying cause of your pain. He or she will be able to help treat your condition in the best way possible.
Proper Foot Care for Diabetic Feet
 Diabetic patients are often aware of the link between foot problems and how their diabetes is managed. Complications can include a numbing sensation or tingling in the feet which may be the beginning of diabetic neuropathy. It may cause the inability to feel existing cuts, wounds, or bruises. If these ailments are left untreated, a diabetic ulcer may form, which may lead to amputation. Additionally, foot muscles may be affected in severely diabetic patients, which may change the alignment of the foot. Proper foot care management can begin with monitoring the glucose levels in the blood. A daily practice of good foot hygiene can consist of washing and drying the feet thoroughly, and special footwear may need to be worn. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can help you to properly manage this condition, in addition to providing you with proper foot care advice.
Diabetic patients are often aware of the link between foot problems and how their diabetes is managed. Complications can include a numbing sensation or tingling in the feet which may be the beginning of diabetic neuropathy. It may cause the inability to feel existing cuts, wounds, or bruises. If these ailments are left untreated, a diabetic ulcer may form, which may lead to amputation. Additionally, foot muscles may be affected in severely diabetic patients, which may change the alignment of the foot. Proper foot care management can begin with monitoring the glucose levels in the blood. A daily practice of good foot hygiene can consist of washing and drying the feet thoroughly, and special footwear may need to be worn. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can help you to properly manage this condition, in addition to providing you with proper foot care advice.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Stephen Petrofsky from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Port Charlotte, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
Diabetes is the condition in which the body does not properly process food for use as energy. People with Type 1 diabetes cannot produce insulin, which is required for glucose to feed your body’s cells. It is typically caused by the immune system mistaking healthy cells for foreign invaders and destroying the insulin-producing cells in the pancreas. On the other hand, people with Type 2 diabetes cannot respond to insulin properly, and eventually cannot produce enough. The Centers for Disease Control and Prevention reports that over 30 million people in the United States have diabetes, with 1 in 4 having no idea they have it. Surprisingly, diabetes is the seventh leading cause of death in the US. The symptoms of diabetes include frequent urination, fatigue, hunger, and even blurry vision.
Diabetes can also affect the feet as well. Over time, diabetes can cause nerve damage to your feet, which could then lead to symptoms such as tingling, pain and numbness in the feet. Neuropathy can be very dangerous to a person with diabetes, since it prevents them from feeling injuries such as cuts or blisters in the feet, and if not detected early enough, may lead to infection. Neuropathy can also lead changes in the shape of your feet and toes. The best way for people with diabetes to prevent or delay neuropathy is keeping their blood glucose levels in their target range. This consists of eating right, having the correct amount of exercise, and taking medications.
Diabetes can also create calluses and foot ulcers as well. Calluses build up faster and occur more frequently with those affected by diabetes. If there are too many calluses, therapeutic shoes and inserts may be required. It is important to have calluses trimmed by a health professional, as doing it yourself may lead to infections. If these calluses continue to develop and thicken, they can lead to foot ulcers. Foot ulcers are open sores, that appear on the ball of the foot or on the bottom of the big toe. These ulcers can lead to future infections if not treated and may possibly result in losing a limb. It is important to report any ulcers to your podiatrist right away. Your doctor may take x-rays to examine the foot and clean out any dead and infected tissue.
Lastly, diabetes can also lead to poor circulation and peripheral arterial disease (PAD). The poor circulation in the feet and leg area is a result of diabetes narrowing and hardening, eventually slowing down the blood flow in that area. The best way to prevent this is to keep away from smoking and follow your doctor’s advice for maintaining blood pressure and cholesterol. PAD is similar to this complication. PAD is when blood vessels narrow or are blocked by fatty deposits. PAD also increases your risk of heart attacks and strokes and is a common condition to those affected by diabetes. The combination of both PAD and neuropathy may lead to infections and can result in amputation of certain limbs. PAD can be prevented with wearing the proper foot wear and regularly taking care of your feet.
If you want to take care of your feet, you should wash and dry them carefully and perform daily inspections to check for cuts, blisters, or swelling. Any physical activity you partake in should be approved by your health care provider. You should also be sure to wear special shoes if advised to do so by your doctor.
The Consequences of a Fall
Falls are the leading cause of injury and hospitalizations in older adults across North America. Most falls occur in the home, due to slipping or stumbling. Falls can result in both minor and major injuries, from bruises and sprains to dislocations and fractures. Injuries sustained from a fall can make falling in the future more likely, as they can impair mobility and decrease an older adult’s self-confidence when it comes to getting around their home and community. There are several steps that you can take to prevent falls, including removing tripping hazards from the home, installing non-slip mats and grab bars in slippery areas, and using a mobility aid when needed. To learn more about preventing falls, please consult with a podiatrist.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Stephen Petrofsky from Florida. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Port Charlotte, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
A Toe Stretch for Plantar Fasciitis
 The plantar fascia is a ligament that runs along the bottom of the foot, and can be at risk of injury. When it is inflamed, usually due to repetitive overuse from playing sports or working out, plantar fasciitis may develop. Symptoms of this condition can include heel pain, arch pain, and possible swelling and tenderness along the bottom of the foot. There are many foot exercises that you can try to help relieve pain. Stretching is one way to help yourself recover from plantar fasciitis. One such exercise is the toe stretch. To do this exercise, sit on the floor with your knee bent and foot flat on the floor. Pull the toes back until you feel a stretch in the arch of your foot. Hold for 30 seconds, and then relax. Repeat 10 times. For more information about plantar fasciitis and foot stretches, please consult with a podiatrist.
The plantar fascia is a ligament that runs along the bottom of the foot, and can be at risk of injury. When it is inflamed, usually due to repetitive overuse from playing sports or working out, plantar fasciitis may develop. Symptoms of this condition can include heel pain, arch pain, and possible swelling and tenderness along the bottom of the foot. There are many foot exercises that you can try to help relieve pain. Stretching is one way to help yourself recover from plantar fasciitis. One such exercise is the toe stretch. To do this exercise, sit on the floor with your knee bent and foot flat on the floor. Pull the toes back until you feel a stretch in the arch of your foot. Hold for 30 seconds, and then relax. Repeat 10 times. For more information about plantar fasciitis and foot stretches, please consult with a podiatrist.
Stretching the feet is a great way to prevent injuries. If you have any concerns with your feet consult with Dr. Stephen Petrofsky from Florida. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Stretching the Feet
Stretching the muscles in the foot is an important part in any physical activity. Feet that are tight can lead to less flexibility and make you more prone to injury. One of the most common forms of foot pain, plantar fasciitis, can be stretched out to help ease the pain. Stretching can not only ease pain from plantar fasciitis but also prevent it as well. However, it is important to see a podiatrist first if stretching is right for you. Podiatrists can also recommend other ways to stretch your feet. Once you know whether stretching is right for you, here are some excellent stretches you can do.
- Using a foam roller or any cylindrical object (a water bottle or soda can will do), roll the object under your foot back and forth. You should also exert pressure on the object. Be sure to do this to both feet for a minute. Do this exercise three times each.
- Similar to the previous one, take a ball, such as a tennis ball, and roll it under your foot while seated and exert pressure on it.
- Grab a resistance band or towel and take a seat. If you are using a towel, fold it length wise. Next put either one between the ball of your foot and heel and pull with both hands on each side towards you. Hold this for 15 seconds and then switch feet. Do this three times for each foot.
- Finally hold your big toe while crossing one leg over the other. Pull the toe towards you and hold for 15 seconds. Once again do this three times per foot.
It is best to go easy when first stretching your foot and work your way up. If your foot starts hurting, stop exercising and ice and rest the foot. It is advised to then see a podiatrist for help.
If you have any questions, please feel free to contact our office located in Port Charlotte, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.